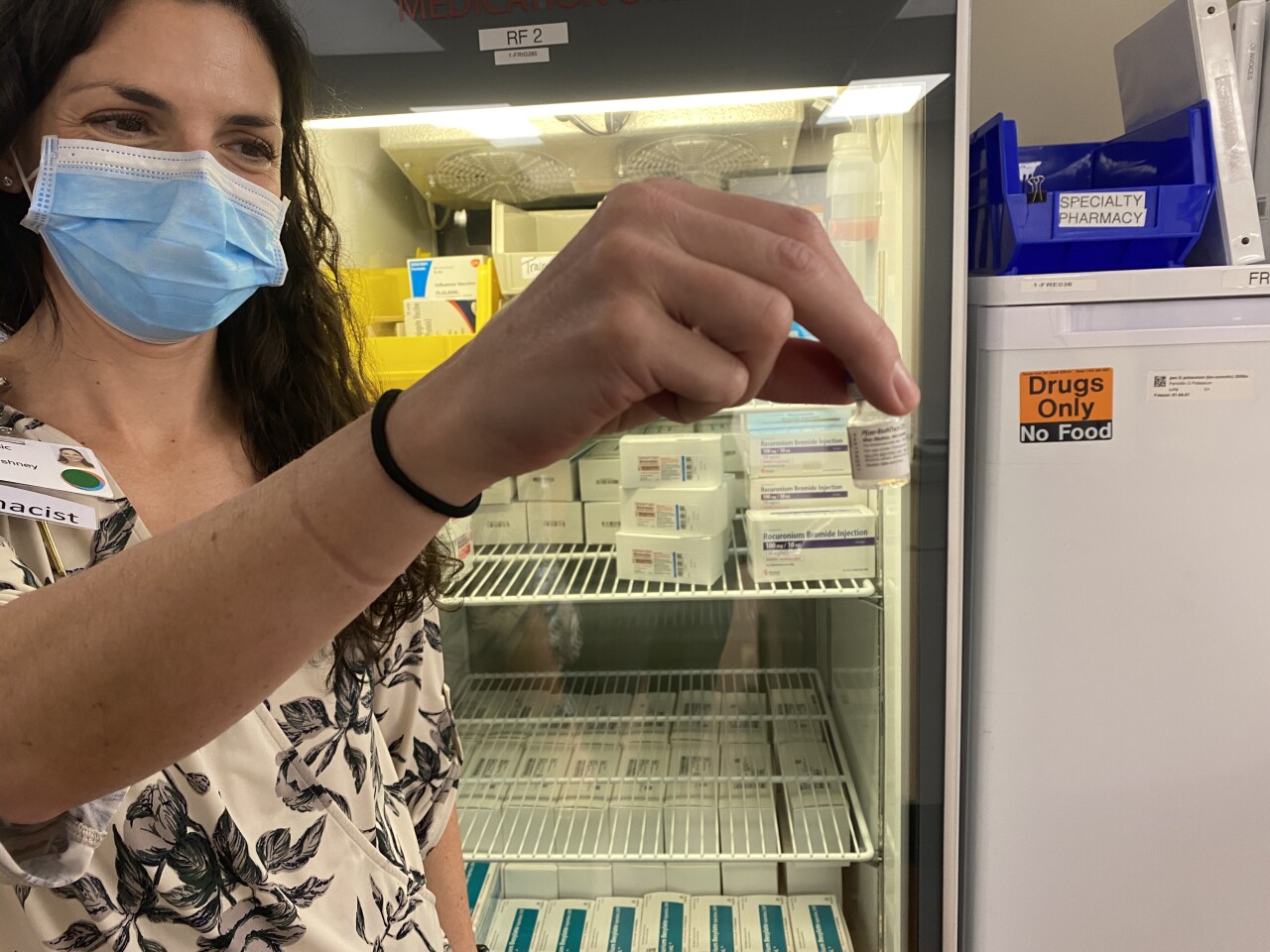
BILLINGS — On Tuesday, five health care workers at Billings Clinic were the first in the city to be injected with the Pfizer COVID-19 vaccine, hopefully signaling a light at the end of the tunnel in the long fight against COVID-19.
The five vaccinated each represented an aspect of the health care system that sees COVID-19 patients. A physician, respiratory therapist, nurse, environmental services staff member and Billings Fire Department paramedic all voluntarily received the vaccine.

The five were injected in the Billings Clinic Commons to an audience of other hospital staff and reporters. While the syringes were filled, Billings Clinic CEO Dr. Scott Ellner thanked the team of pharmacists, pharmacy techs, physicians, nurses, security staff and facilities planning staff for their work in securing the new drug.
"We’ve worked tirelessly to get the vaccine in really record time. I am feeling so blessed and optimistic that in the next few months as we distribute the vaccine to our health care workforce, we’re going to see a light coming out of this fog and continue to give care like we always have in an environment where people feel safe," Ellner said.
After Ellner, Dr. Toni Green, chief medical officer at Billings Clinic, took the podium to deliver remarks, thanking all hospital staff for their service.
"We’re very proud of our health care workers and their service they provide relentlessly, without pause over the last several months and knowing there’s a light at the end of the tunnel to this pandemic gives us all amazing hope," Green said.
Billings Clinic received 975 doses of the Pfizer COVID-19 vaccination. On Wednesday, a small group of hospital staff will be vaccinated to ensure proper procedures are in place, Green said. Then on Thursday, a wider, voluntary distribution effort will start among the health care workers.

Once the initial shipment runs out, the hospital will have to ask the state for more, with the goal to eventually distribute the vaccine to the public, Green said.
"The state is on an allocation schedule and we’ll be able to continue those vaccinations not only at Billings Clinic, with also family medicine residency for RiverStone (Health), our anesthesia partners and continue to expand that to the community as soon as we have enough allocation available," Green said.
It will be some time before a vaccine is available for rural, critical access hospitals, Green said.
The rural hospitals aren't able to store the Pfizer vaccine, due to it's cold storage requirement of -70 degrees Fahrenheit. Green said the rural hospitals will have to wait for the vaccine manufactured by Moderna, which can be stored in a conventional freezer at -4 degrees Fahrenheit.
The Moderna vaccine's application with the U.S. Food and Drug Administration is expected to be reviewed on Dec. 17, with a roll out expected before the end of the year, according to CNN.

As for how the vaccine works to prevent COVID-19, Green broke it down in simple terms. Essentially, the vaccine helps trigger the immune system to identify COVID-19 as something foreign to the body, building an immune response. The Pfizer vaccine requires a second dose 21 days later, thus increasing the immune response, Green said.
"That’s part of the importance of the second shot, to kind of super-enforce that (immune response) in your cells, if you will. Then (your body) knows to fight that so if you do get exposed to the virus later, your body has built up its ability to fight (COVID-19),” Green said.
Green said that a vaccine is not a cure. A vaccine serves to prevent a disease, while a cure means that you can eradicate the disease. She used the example of the smallpox virus, which isn't seen much due to widespread vaccination, but still pops up in patients occasionally.
"Smallpox for example, we’ve had a vaccine for many years, so in essence you think it’s cured. However, we do see it show up every once in a while. It can be confusing but a vaccine prevents a disease from occurring. A cure means we have killed it completely and that is not what the vaccine is geared for," Green said.
Michelle Buffington was the respiratory therapist who received the vaccine. Buffington said said she hopes the vaccine will lift the spirits of health care workers who've been struggling through long shifts to care for the high number of patients in the hospital.
“I think as health care providers we’re kind of at that point where we’re all just exhausted, physically, emotionally. I think everybody is kind of ready to move on and somebody has to start it," Buffington said.
As a respiratory therapist, Buffington has been on the front line monitoring and rationing ventilators for COVID-19 patients who sometimes have a six-week stay in the hospital for more severe cases.
“You’re trying to go in there and tell them that it is going to be okay, but for some of them it’s not. It’s pretty heart breaking," Buffington said.
Buffington said she was nervous to receive the brand new drug, but the fear of the vaccine wasn't as severe as the results she's seen in COVID-19 patients.
“I think (the vaccination is) not as scary as getting COVID-19. We’ve got to start somewhere and all I can say is wear your masks, COVID-19 is real. A lot of people still think that it is not, but it is. It’s pretty devastating to people that get it," Buffington said.

Another person in the group to receive the vaccine was Jason Banfield, Billings firefighter and paramedic. He said the actual poke of the needle was just the same as his annual flu shot.
"It was super easy. It felt like a flu shot. I got my flu shot this year. I think it's important that people kind of lean forward and look at the whole group of our population. We just need to take care of each other, and this is one way that we can do that," Banfield said.
Banfield said his family was one reason for getting the vaccine. He helps his 96-year-old grandmother with her groceries and wanted to keep her safe along with his mother who has cardiac issues, Banfield said.
With his line of work as a first responder, Banfield said he also got the vaccination to keep his patients safe.
“I can’t be the one that brings this into your home. Also if you are a trauma patient and I have to extricate you out of a vehicle and then I add COVID-19 to your problems as a trauma patient, that is not what we’re here for," Banfield said.
Another problem Banfield encounters as a first responder: he often doesn't know if he's interacted with a COVID-19 positive patient until after the fact, making his vaccination more important.
“The level of personal protective equipment that we have to use going into unknowns, trying to figure out who is COVID-19 positive home or getting that information has been critical in how we do business. We’re out there taking care of those patients before they come to the hospital," Banfield said.
The vaccine will also help keep more first responders working on the streets, Banfield said. At a certain point, it is hard to run a fire department if a majority of the staff is quarantined or ill.
“We’re a limited group of people, just like nurses and physicians, firefighters and police officers. You only have so many, if you take out 20 or 30 percent of that population because they are home sick, you have limited services for you and the public when you dial 9-1-1," Banfield said.
Above all, Banfield said he's hopeful for the day when the community reaches herd immunity when a majority of the population is vaccinated.
"We need to make sure that we are doing the best and that we’re not part of the problem and that we’re part of the solution. If we can get our herd immunity up in the hospital sense and also the prehospital, that helps with the care," Banfield said.
RELATED: Bullock joins St. Vincent Healthcare for administering of first doses of Pfizer vaccine